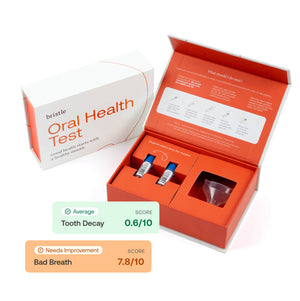
Background
90% of bad breath is caused by specific bacteria in the oral cavity, also known as the oral microbiome. These bacteria create dozens of foul smelling compounds such as hydrogen sulfide, methylmercaptan, putrescine, and cadaverine. The production of these foul smelling compounds is often a sign of oral microbiome dysbiosis, oral disease, or poor oral hygiene. Many of the bacteria that create these compounds are associated with periodontal disease, a progressed stage of gum disease characterized by irreversible bone loss and gum inflammation.
What causes persistent bad breath?
The vast majority (90+%) of all cases of persistent bad breath are caused by bacteria in the mouth, which are members of a community of microbes also known as the oral microbiome. Many of the microbes that cause bad breath are anaerobic bacteria that also are implicated in gum disease. These bacteria form a biofilm at the gumline which is notoriously difficult to remove. As inflammation causes tissue damage, the biofilm grows deeper into the periodontal pocket, causing more damage, creating a feedforward loop. As disease progresses, disease becomes irreversible through bone loss and deep periodontal pockets that require constant maintenance or surgery.
These anaerobes ferment the proteins in saliva and from diet that result in foul smelling byproducts such as hydrogen sulfide, putrescine, cadaverine, and propionic acid. The accumulation of these bacteria and foul smelling compounds causes persistent bad breath. While hygiene habits like flossing and tongue scraping have been shown to reduce anaerobic species, they are often short-lived solutions as the bacteria that cause bad breath grow back rapidly, especially in cases of existing oral disease.
Other microbes that live on the tongue, such as Solobacterium moorei, can also cause persistent bad breath. These bacteria form a biofilm in the crypts of the back of the tongue, where they are extremely difficult to remove. Solobacterium moorei is in approximately 25-50% of all people, and causes bad breath through metabolism of proteins in saliva and lingering food particles, generating foul smelling volatile sulfur and volatile organic compounds. Often, the use of antimicrobial mouthwashes is insufficient to remove this species, though supplementation with nitrate has been shown to reduce levels of anaerobic species.
Prevention, and maintenance of oral hygiene and the oral microbiome, is usually the best measure at reducing potential periodontal pathogens from permanently wreaking havoc on your oral health and oral microbiome.
So, is halitosis contagious?
In short, yes, the bacteria that cause bad breath are contagious.
Bacterial species in the oral microbiome are definitely transmitted from person to person. Direct mucosal contact through kissing is the most probable route of transmission, but saliva contact or droplets cannot be ruled out. Additionally, commensal bacteria are readily shared between people. Pathogenic species transmission happens most common with people who already have existing oral disease, as they harbor the highest abundance of those pathogenic species. Here are the studies that support the conclusion that microbes that cause bad breath are transmitted from person to person:
Transmission of human-associated microbiota along family and social networks
The authors leveraged a unique dataset from Fiji (http://fijicomp.bme.cornell.edu/), where participants shared their familial and social networks and interpersonal relationships. They also sequenced the gut and oral microbiomes by shotgun metagenomic sequencing from each of the 287 participants. They found that bacterial strains in the oral microbiome are readily shared among social networks, and in some cases there is “supersharing” where there are significantly higher shared oral microbiome strains among pairs of people, indicating higher than usual transmission.
Horizontal Transmission of Mutans Streptococci in Children
Bacteria were isolated from the mouths of schoolchildren and cultured on media that selects for Streptococcus species, specifically Streptococcus mutans. The authors used a genotyping technique called arbitrarily primed PCR to look at the strains of bacteria from each of the children. They found that pairs of children that were not siblings shared the same genotype of S. mutans, demonstrating transmission between children that shared a classroom.
This review summarized dozens of transmission studies looking at transmission of these two periodontal pathogens in families. They found a transmission rate of 14-60% for Aggregatibacter actinomycetemcomitans, and 30-75% for P. gingivalis.
The authors studied spousal pairs, and performed traditional microbiological culturing to identify strains of A. actinomycetemcomitans and P. gingivalis in 11 spousal pairs. 4 of 11 spousal pairs shared the same A. actinomycetemcomitans strain, demonstrating horizontal transmission. Interestingly, 7 of the remaining pairs carried varying strains of A. actinomycetemcomitans, either indicating intra-host evolution or a separate transmission event that exposed them to A. actinomycetemcomitans.
Transmission of Porphyromonas gingivalis between spouses
Bacteria were isolated from the mouths of 10 spousal pairs. P. gingivalis was detected in 8 pairs, and absent in the other two. In 6 of the 8 pairs with P. gingivalis, authors used restriction fragment length polymorphism analysis to determine that the strains were indistinguishable from one another. This study demonstrated that P. gingivalis was readily transmitted between spouses.